
The year 2026 marks a demographic milestone we've been anticipating for decades: the oldest baby boomers are turning 80.
Over the next 20 years, 73 million boomers will pass through their 80s — a period when care needs intensify dramatically. By 2034, for the first time in U.S. history, more Americans will be over 65 than under 18. This isn't a prediction anymore. It's happening now.
So here's what actually matters for senior care in 2026, backed by hard numbers from AARP, Grand View Research, Deloitte, the Alzheimer's Association, and other organizations that measure real-world adoption and spending.
Top Senior Care trends going into 2026:
- Aging in place goes mainstream — 84% of Americans 50+ prefer to stay home
- AI-powered predictive health monitoring — AI predicts Alzheimer's with 78% accuracy years before symptoms
- Remote patient monitoring explodes — $56.9B market by 2030, 142M U.S. patients using RPM by 2030
- The caregiver crisis hits critical mass — 4.6M unfilled jobs projected by 2032
- Smart home tech for seniors — Smart home ownership tripled from 10% (2019) to 27% (2024)
- Telehealth becomes standard senior care — 25% of Medicare beneficiaries used telehealth in 2024
- Memory care gets a complete redesign — 7.2M Americans living with Alzheimer's, $360B annual care cost
- Seniors embrace AI tools — AI usage among 50+ nearly doubled from 18% to 30% in one year
- Unified care platforms replace fragmentation — 70% of home healthcare patients are 65+
- Intergenerational living communities emerge — New village-style developments blending age groups
- Regulatory expansion and enhanced oversight — 18 states updated assisted living regulations in 2025
- Workforce innovation tackles staffing — 99% of nursing homes have open positions
Let's get into it.
1. Aging in Place Goes Mainstream — And the Market Is Responding
The numbers are unambiguous. According to AARP's 2026 Tech Trends survey, 84% of Americans over 50 want to age in place — staying in their own homes rather than moving to assisted living or nursing facilities.
This isn't just preference. It's becoming infrastructure.
The AgeTech market — dedicated to developing tools that help older adults live independently at home — is projected to reach $120 billion by 2030, according to AARP research. And companies are racing to capture that spend.
The elderly care market globally is projected to grow from $53.29 billion in 2025 to $114.57 billion by 2034 — a 9% CAGR driven almost entirely by home-based care solutions rather than institutional settings.
What's happening in the real world
Home Instead and similar home care franchises are expanding rapidly, offering bundled packages that combine home retrofits, visiting nurses, and social programs. The model delivers "community without relocation" — seniors get social connection and medical support without leaving their homes.
Best Buy Health acquired Current Health and is positioning itself as a major player in home-based monitoring. Their strategy: leverage existing retail infrastructure and Geek Squad support to deploy and maintain health technology in seniors' homes.
Amazon offers Alexa Emergency Assist, a subscription service specifically designed for aging in place. It includes fall detection, emergency helpline access, and remote check-ins for family caregivers — all voice-activated for seniors who may struggle with smartphone interfaces.
Where this is heading
2026 is the year aging in place stops being an alternative and becomes the default assumption.
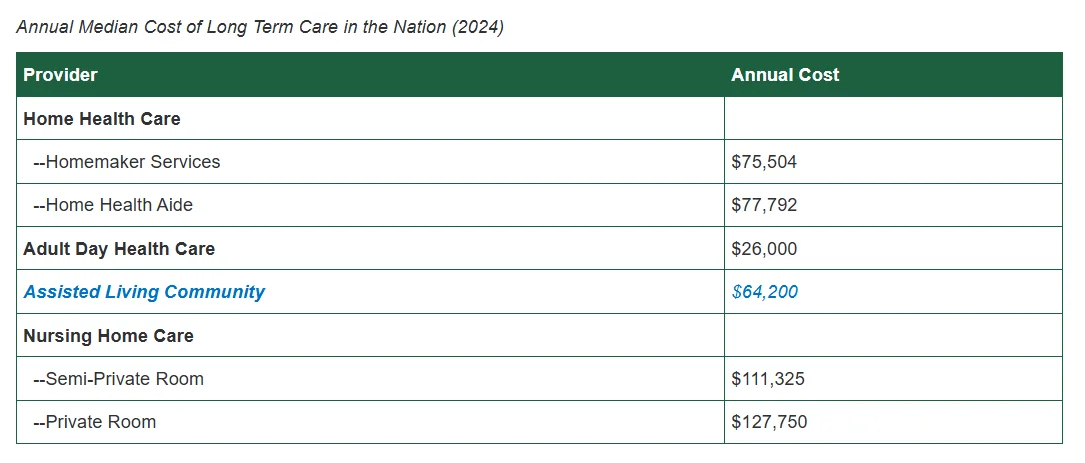
The economics make sense: institutional care costs $5,350/month median for assisted living, according to NCAL data. Home-based care with technology support can cost a fraction of that while delivering outcomes seniors actually prefer.
Expect massive growth in home modification services — grab bars, walk-in tubs, stair lifts, wider doorways. The boring infrastructure of aging in place is suddenly a growth industry.
2. AI-Powered Predictive Health Monitoring Changes Everything
This is the trend that could fundamentally reshape geriatric care: AI systems that predict health crises before they happen.
According to research published in BMC Geriatrics, AI-driven tools including machine learning algorithms, predictive analytics, and assistive robotics are increasingly utilized to address challenges associated with aging — frailty, multimorbidity, polypharmacy, and fall prevention.
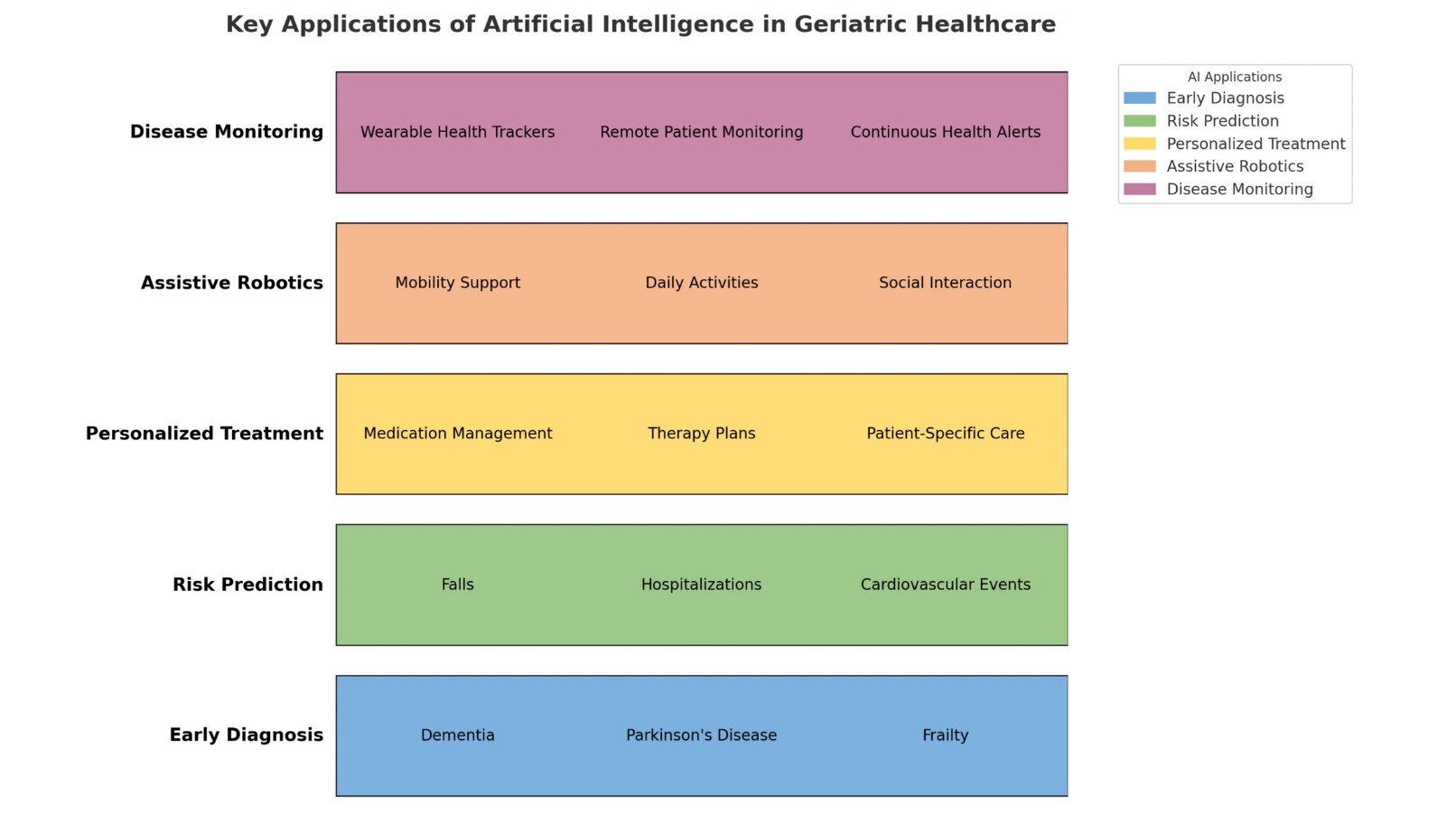
The breakthrough that caught everyone's attention: researchers developed a speech-analysis AI model capable of predicting Alzheimer's progression with 78.5% accuracy."
Mass General Brigham developed an AI that can forecast cognitive decline and eventual dementia years before symptoms start.
Fall prediction is getting similarly sophisticated. One study developed an ML-based fall prediction model for nursing home residents that predicts fall occurrences within six months after baseline assessment — giving staff time to intervene.
What's happening in the real world
Google Health is deploying AI systems that analyze electronic health records to identify patients at risk of deterioration. Their models combine lab values, vital signs, and clinical notes to surface concerns that human reviewers might miss.
Biofourmis uses continuous wearable monitoring combined with AI to detect early signs of heart failure decompensation. Their algorithms learned patterns from thousands of patients, recognizing subtle changes that precede hospitalizations.
CarePredict offers AI-powered senior care that learns each individual's patterns — walking speed, sleep quality, eating habits — and alerts caregivers when deviations suggest potential health issues.
Where this is heading
The promise is shifting from reactive to preventive care. Instead of responding to falls, we prevent them. Instead of treating advanced dementia, we intervene years earlier when treatments are more effective.
But adoption faces real barriers. According to research, only 48% of those aged 80+ believe they have the digital skills necessary to take advantage of being online.
The technology is advancing faster than seniors' comfort with it. (For more on how AI is transforming healthcare delivery across all demographics, see our generative AI trends for 2026.)
3. Remote Patient Monitoring Explodes Into the Mainstream
Remote patient monitoring (RPM) has moved from pandemic necessity to standard care infrastructure.
According to MarketsandMarkets, the global RPM market was valued at $24.39 billion in 2023 and is projected to hit $56.94 billion by 2030 — a 12.7% CAGR. The U.S. market alone has now exceeded $18 billion in 2026.
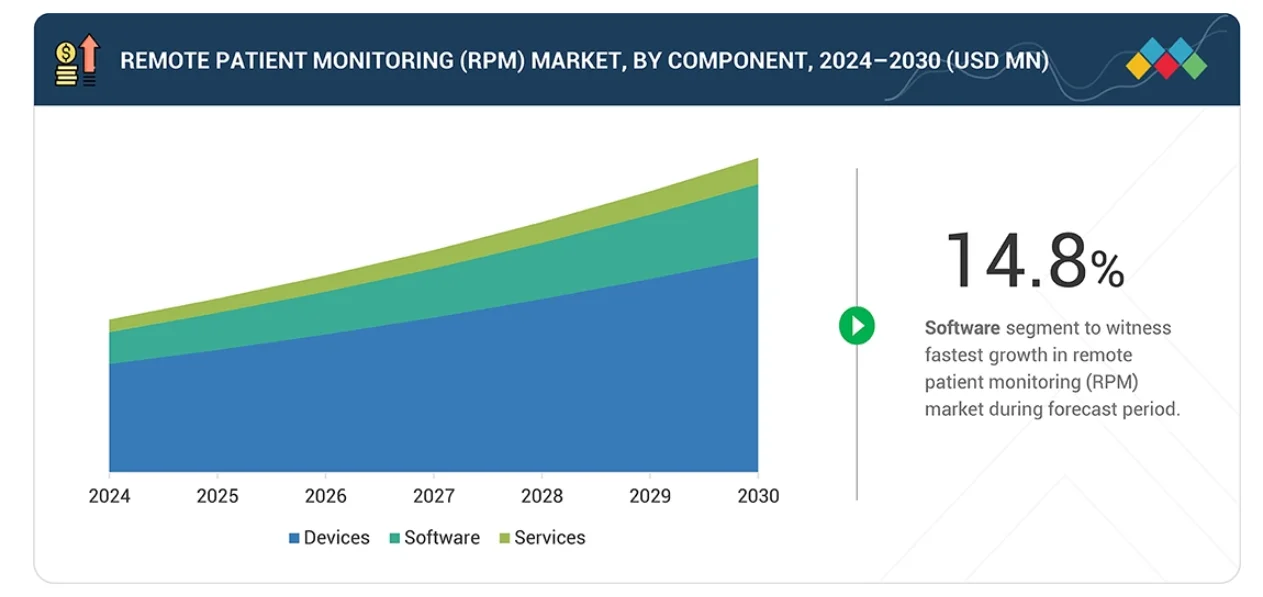
Source: MarketsandMarkets Remote Patient Monitoring Market Report 2025
The adoption numbers are staggering. According to IQVIA projections, over 142 million U.S. patients — nearly 40% of the population — will be using RPM technologies by 2030. And the elderly are the primary users: 70% of home healthcare patients are 65 years of age and above.
Grand View Research reports that North America dominates with 40.53% market share in 2024, driven by advanced healthcare infrastructure and the presence of leading RPM solution providers.
What's happening in the real world
Livongo (now part of Teladoc) pioneered the connected glucose monitor for diabetics, sending real-time data to care teams. Their model — hardware plus AI plus human coaches — became the template for chronic disease management.
Philips expanded its hospital-at-home programs, deploying monitoring equipment that tracks vitals continuously while patients recover at home instead of in beds that cost $2,000+ per night.
Hungary's government launched a Remote Health Monitoring Programme funded by the EU with EUR 229 million, providing wearable sensory devices to more than 1.5 million seniors for 24-hour monitoring plus emergency medical services.
Where this is heading
Medicare coverage is the accelerator. In 2026, Medicare broadly covers home health nursing, physical therapy, occupational therapy, and medical social services — including certain telehealth consultations and some remote patient monitoring devices.
The devices themselves are disappearing into everyday objects. Watch-based monitoring. Bed sensors. Smart scales.
The goal is ambient health awareness without seniors having to do anything different. (For a deep dive into the broader wearable health monitoring revolution, see our wearable technology trends for 2026.)
4. The Caregiver Crisis Hits Critical Mass
Here's the number that should alarm everyone: there will be 4.6 million unfulfilled caregiving jobs by 2032.
The direct care workforce comprises 5.4 million workers today, according to PHI National — including nearly 3.2 million home care workers, over 687,000 workers in residential care homes, and more than 492,000 nursing assistants in nursing homes.
But demand is exploding. Between 2024 and 2034, the direct care workforce is projected to need 9.7 million total jobs filled — including new positions and replacements for workers who leave. That's the largest growth of any job sector in the country.
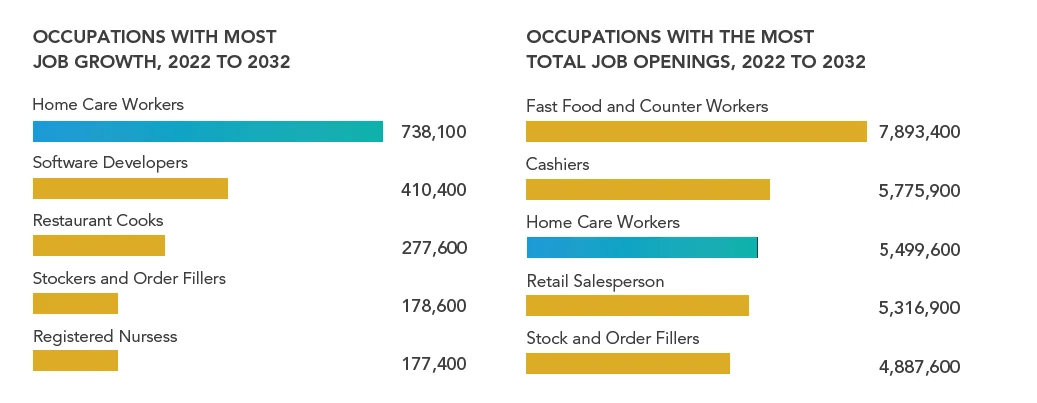
The crisis is already here. According to AHCA/NCAL surveys, 99% of nursing homes and 96% of assisted living facilities are facing staffing shortages. Two-thirds of nursing homes report that ongoing shortages may require them to close.
What's happening in the real world
Honor raised $140 million to build technology that makes caregiving more efficient. Their platform handles scheduling, matching, and administrative burden — letting caregivers spend more time on actual care.
CareAcademy provides online training and certification for caregivers, creating career ladders that didn't exist before. The logic: if you can't hire enough people, make each person more capable.
Several states are experimenting with immigration reforms specifically targeting healthcare workers. The argument gaining traction: "You've either got to pay more, or you've got to let in way more people."
Where this is heading
The math is brutal. From 2022 to 2060, adults age 65+ will increase from 57.8 million to 88.8 million. Adults 85+ will nearly triple from 6.5 million to 17.5 million. Demand will outpace supply for decades.
Technology will help but won't solve it. AI can handle documentation. Robots can assist with lifting. But human connection — the core of caregiving — can't be automated. The organizations that figure out how to attract, retain, and develop caregivers will have massive competitive advantages.
5. Smart Home Technology Becomes Standard Senior Care
Smart home adoption among seniors has tripled in five years.
According to AARP research, smart home technology ownership among those 50+ grew from 10% in 2019 to 27% in 2024. Voice assistants, medical alert systems, and AI-powered sensors are now mainstream products — not tech experiments.
The global smart home market is projected to reach $231.6 billion by 2028, with seniors representing one of the fastest-growing customer segments.
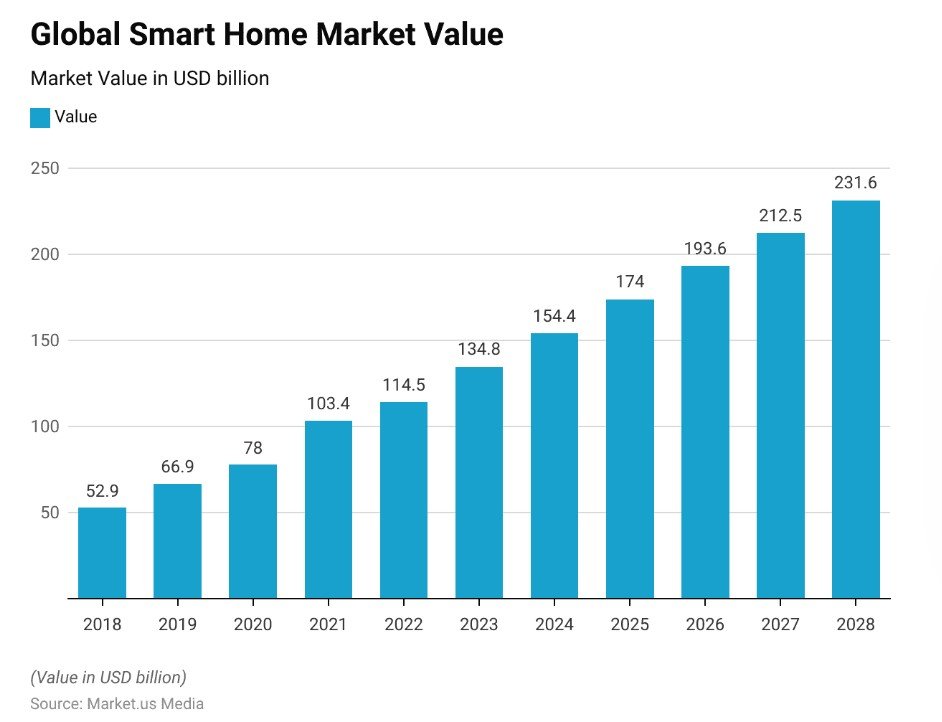
The AgeTech Collaborative reports that motion detectors, fall-detection devices, and voice-activated assistants are creating safer home environments across millions of households.
What changed? The technology got easier. Voice interfaces mean seniors don't need to navigate smartphone apps. Installation services mean they don't need tech skills. And family caregivers can monitor remotely, extending their ability to help from anywhere.
What's happening in the real world
Amazon Alexa has become the de facto voice platform for senior care. More than a third of Americans own a smart speaker, and seniors use them for medication reminders, emergency calls, entertainment, and controlling lights and thermostats — all hands-free.
Apple Watch added fall detection, irregular heart rhythm alerts, and emergency SOS features specifically targeting older users. The device went from fitness tracker to medical device.
SimpliSafe and similar security companies now market directly to seniors and their adult children, offering monitoring systems that detect unusual activity patterns — a door that doesn't open in the morning, for instance.
Where this is heading
Privacy-respecting alternatives are emerging.
According to Helpany, AI-driven camera-free systems can understand what a resident needs without ever capturing an image. "This is the real promise of AI: We no longer need cameras or audio to understand what a resident needs."
The biggest barrier remains mindset. Nearly six in 10 (59%) older adults don't believe today's technology is designed with them in mind, according to AARP research. That's a design problem, not a market problem.
6. Telehealth Becomes Standard Senior Care
Telehealth usage among seniors has stabilized at levels that would have been unthinkable pre-pandemic.
According to Medicare data, 25% of Medicare fee-for-service users had a telehealth visit in 2024 — roughly the same as 2023.
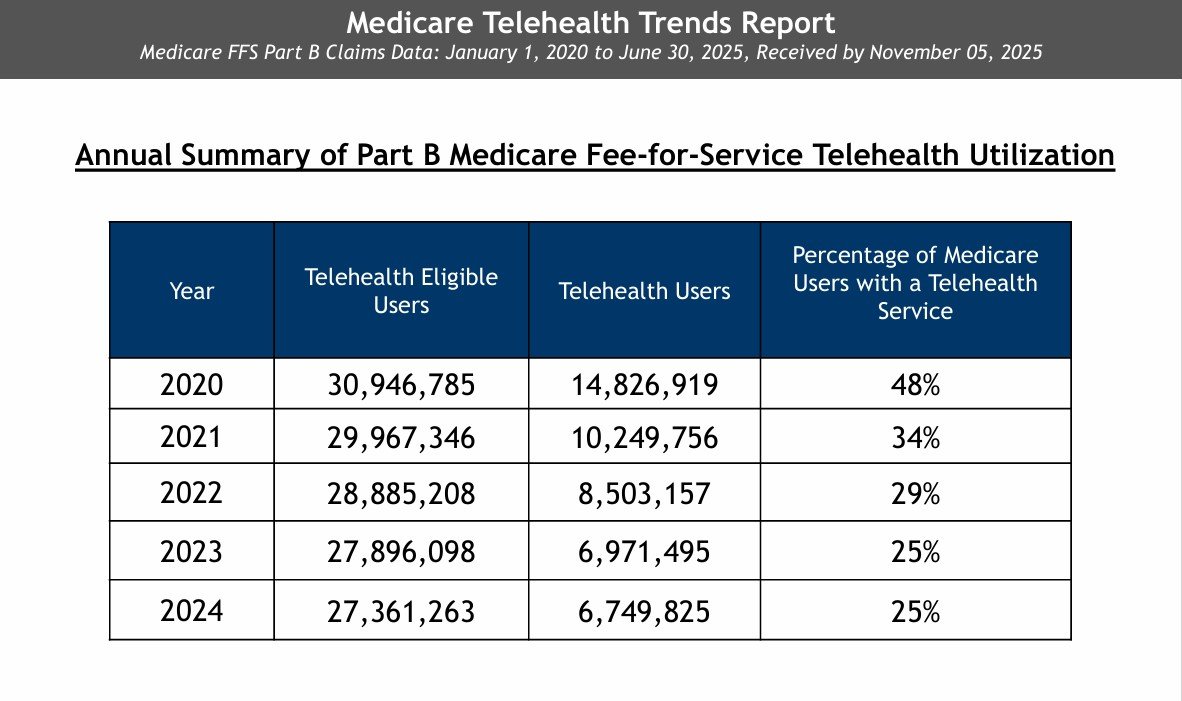
During the pandemic peak, Medicare telehealth visits increased 63-fold compared to 2019. We're not going back.
For those aged 70+, telehealth use increased to 21.1% from 4.6% pre-pandemic — a fundamental shift in how older adults access healthcare. Nearly 3 million Medicare beneficiaries used telehealth in the first quarter of 2024 alone.
The policy support is in place. The Consolidated Appropriations Act, 2026, signed in February 2026, extended Medicare telehealth flexibilities through December 31, 2027, including audio-only options for seniors without video capability and expanded provider eligibility.
What's happening in the real world
Teladoc Health serves millions of Medicare Advantage members through partnerships with major insurers. Their senior-focused offerings include longer appointment times and simpler interfaces designed for older users.
Amwell partnered with Google Cloud to build telehealth infrastructure that hospitals can deploy quickly. Their senior care modules include medication management and chronic condition monitoring integrated with virtual visits.
Dispatch Health combines telehealth with in-home visits — a hybrid model where complex cases get video consultation with a physician while a paramedic-level provider is physically present.
Where this is heading
Audio-only telehealth — basically phone calls with your doctor — turns out to be crucial for seniors. Video requires reliable internet, devices with cameras, and technical confidence. Phone calls require none of that, and Medicare now covers them through 2027.
Congress extended the flexibilities through December 2027, but the industry continues lobbying aggressively to make the changes permanent rather than requiring repeated last-minute extensions.
7. Memory Care Gets a Complete Redesign
The scale of the dementia crisis is staggering.
According to the Alzheimer's Association, an estimated 7.2 million Americans aged 65 and older were living with Alzheimer's dementia in 2025.
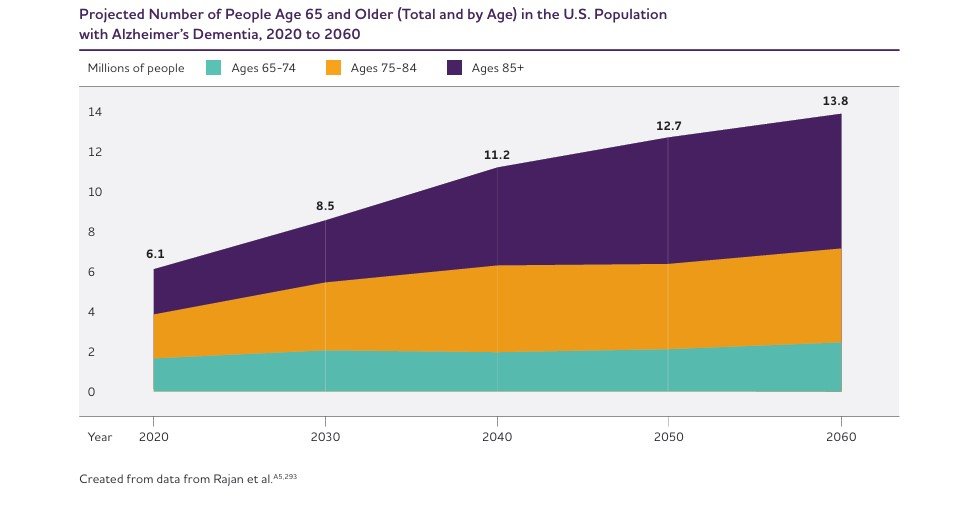
The total national cost of caring for individuals with Alzheimer's and other dementias reached $360 billion in 2024.
Globally, according to WHO data, approximately 55 million people have dementia, with almost 10 million new cases reported every year. Projections show dementia cases reaching 78 million by 2030 and 139 million by 2050.
The memory care market is responding with innovation. The Alzheimer's therapeutics industry has reached $6.2 billion in 2026 and is projected to hit $13.13 billion by 2035.
What's happening in the real world
Eli Lilly's Kisunla (donanemab) received FDA approval in July 2024 for adults with early symptomatic Alzheimer's disease. It's one of a new class of drugs that target the underlying disease mechanism, not just symptoms.
Eisai and Biogen's LEQEMBI (lecanemab) now has FDA acceptance for a subcutaneous autoinjector — making administration at home feasible instead of requiring IV infusions at medical facilities.
Memory care facilities are redesigning physical spaces based on research. Layouts now feature safe wandering paths, calming color schemes, and secured indoor/outdoor access. The goal: minimize confusion and agitation while fostering autonomy.
Where this is heading
AI diagnostics are advancing rapidly.
In a study recently published in BMC Geriatrics, researchers developed speech-analysis models capable of predicting Alzheimer's progression with 78.5% accuracy. Mass General Brigham's AI forecasts cognitive decline years before symptoms start. Earlier diagnosis means earlier intervention.
According to Mordor Intelligence, over 25 molecules are currently in late-stage clinical trials targeting Alzheimer's from early-stage to severe cases. The treatment landscape in 2030 will look nothing like today.
8. Seniors Embrace AI Tools — Faster Than Expected
Here's a stat that surprised the researchers: AI usage among adults 50+ nearly doubled in one year — from 18% in 2024 to 30% in 2025.
According to AARP Tech Trends data, the shift is real. Two-thirds of adults 50+ (66%) now agree that technology enriches life and makes aging easier. Among those 80+, the share agreeing that technology enables a healthy life rose from 39% in 2024 to 46% in 2025.
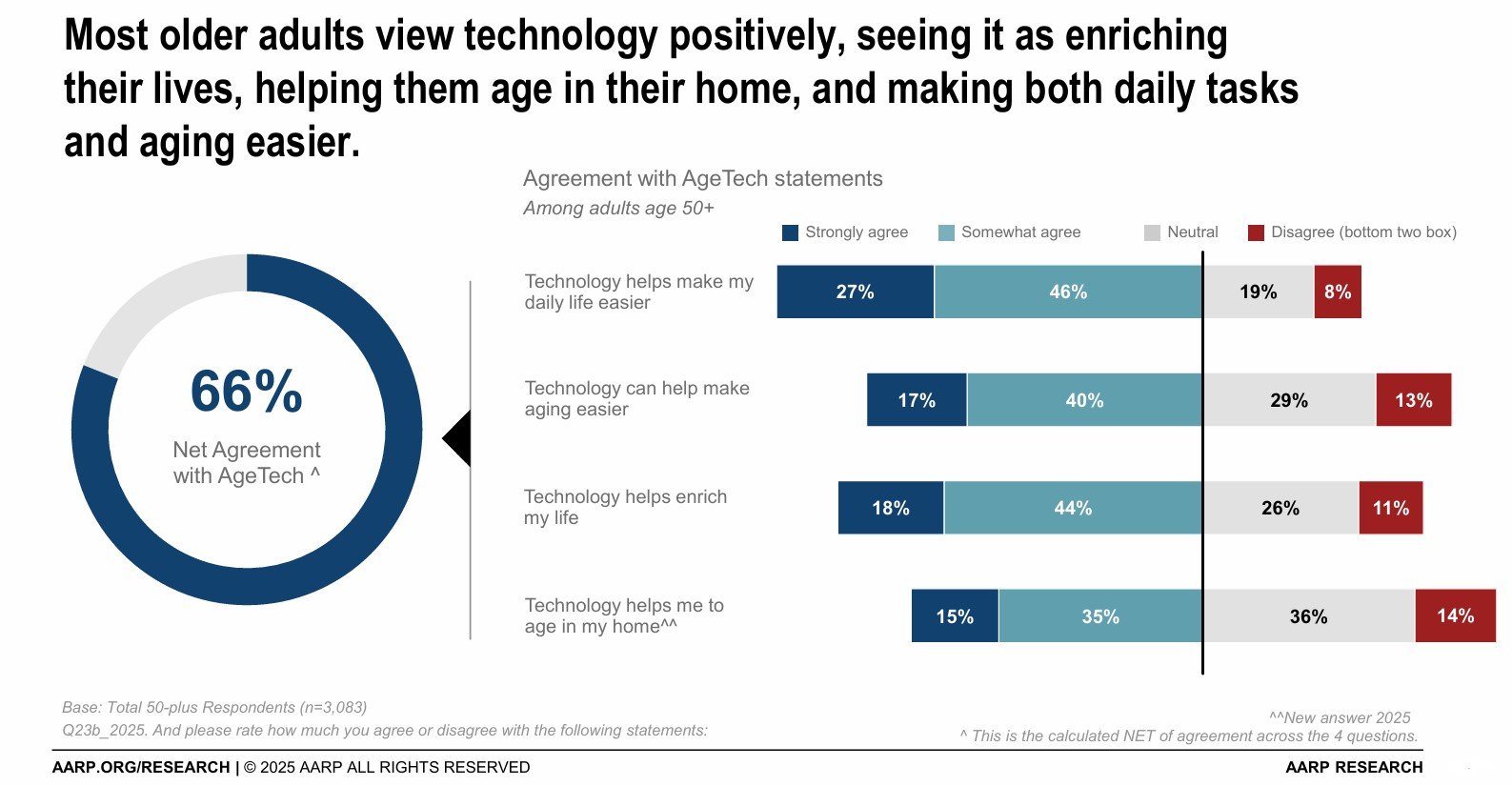
Tech purchasing is accelerating. 71% reported buying technology in 2025, up from 67% in 2024. Two in five are already planning tech purchases for 2026. On average, older adults spent $756 on technology last year.
But barriers remain. Data privacy concerns are the biggest obstacle, cited by one-third of older Americans. Ease of use (20%), setup and support (19%), and cost (16%) follow.
What's happening in the real world
ChatGPT usage among seniors is growing for practical tasks — writing emails, summarizing articles, getting explanations of medical terms. The conversational interface works better than traditional search for many older users.
Voice assistants are the gateway drug. Once seniors get comfortable asking Alexa for the weather, they start using it for reminders, calls, and smart home control. The learning curve is gentler than smartphones.
Family tech support is evolving. Adult children set up devices and accounts, then provide remote support when problems arise. The infrastructure for helping seniors with technology is becoming formalized.
Where this is heading
The gap is still real. Only 48% of those aged 80+ believe they have the digital skills necessary to take advantage of being online. And 66% of those aged 80+ think tech was not designed with them in mind.
2026 is the year companies either figure out senior-friendly design or lose a massive market. The winners will build for cognitive accessibility, not just visual accessibility.
9. Unified Care Platforms Replace Fragmentation
The most frustrating aspect of senior care is the fragmentation. Different systems for the doctor's office, the pharmacy, the home care agency, the insurance company. Nothing talks to anything.
2026 marks a decisive shift. According to Senior Housing News, "Communities are now seeking one unified platform that accompanies residents across the entire continuum of care — a single solution that grows as needs grow."
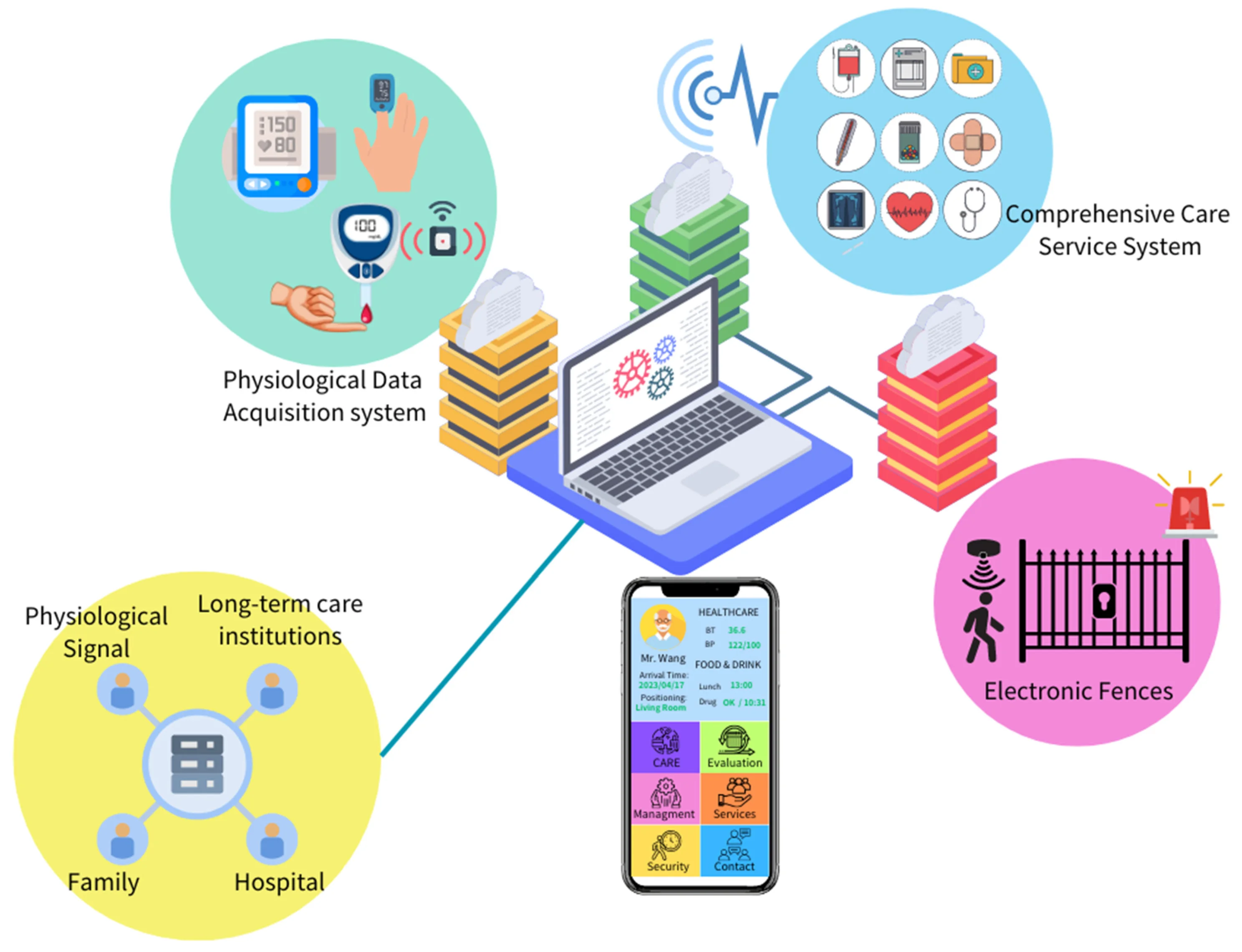
Source: Al-Rousan et al., "Integrating Artificial Intelligence and Wearable IoT System in Long-Term Care Environments." 2023
The market is responding. According to market analysis from Coherent Market Insights regarding the elderly care market, telehealth and remote monitoring represents the leading technology integration segment, capturing 40.2% of elderly care market share in 2025.
The driver is simple: 70% of home healthcare patients are 65 years of age and above, according to market research. When one population dominates a market this completely, platforms optimize for that population.
What's happening in the real world
Epic's MyChart is becoming the de facto patient portal for seniors, with growing integration across hospitals, specialists, and pharmacies. Seniors and their caregivers can see appointments, results, and medications in one place.
CareLinx (acquired by Sharecare) connects families with caregivers while integrating care coordination, billing, and communication in a single platform.
Medisafe turns medication management into a family affair — seniors get reminders, caregivers get alerts about missed doses, and doctors get adherence data.
Where this is heading
The vision is a "digital health passport" that follows seniors across all their care settings — from home to hospital to rehab to home again. Each transition point is where errors happen. Unified platforms reduce those errors.
The challenge is interoperability. Healthcare systems have invested decades in incompatible technologies. Breaking down those walls requires both technical standards and business incentives to share data.
10. Intergenerational Living Communities Emerge
Here's a quiet revolution: seniors don't want to live only with other seniors.
According to Saving Advice, integrated community-based living is gaining momentum in 2026. Steve Nygren, founder of Serenbe, explains: "As a cohort, boomers are very active. As part of their active lifestyles, they're seeking accommodations that incorporate intergenerational living."
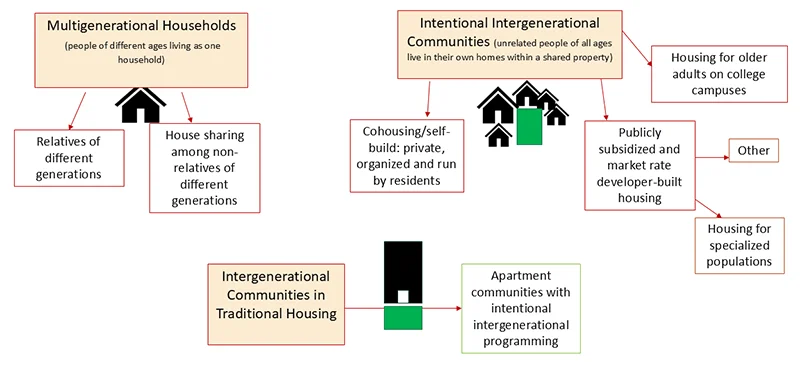
In 2026, Serenbe will start constructing a village-style community with 97 units that blend age groups. This isn't assisted living with young visitors — it's intentional design where different generations live as neighbors.
The model addresses multiple problems simultaneously: seniors get social connection across age groups, younger residents get affordable housing, and the community builds natural support networks.
What's happening in the real world
Nesterly matches older homeowners with young renters, typically college students or young professionals. The senior gets rental income and companionship; the renter gets affordable housing.
The Village Movement has grown to over 350 member organizations nationwide — grassroots networks where neighbors help neighbors age in place, with intergenerational participation baked in.
Co-housing communities designed for mixed ages are proliferating, particularly in progressive urban areas. The waiting lists for many projects extend for years.
Where this is heading
The traditional trajectory — independent living to assisted living to nursing home — is being questioned. What if the goal isn't segregating people by age and ability, but integrating care into normal communities?
The economics work when you share infrastructure. One community kitchen, one fitness facility, one transportation service — scaled across multiple households rather than replicated in each assisted living facility.
11. Regulatory Expansion and Enhanced Oversight
Senior care is getting more regulated — and that's probably a good thing.
According to the National Center for Assisted Living's 2025 Regulatory Review, 18 states (including the District of Columbia) updated assisted living regulations between January 1, 2025, and December 31, 2025.
The top areas for regulatory changes: Direct Care Staff Education and Training Requirements (10 states, 20%), Administrator/Director Education and Training Requirements (9 states, 18%), and Staff Scheduling Requirements (7 states, 14%).
Following the repeal of federal staffing ratios in late 2025, the focus has shifted from national numerical mandates to state-level transparency and acuity-based scheduling.
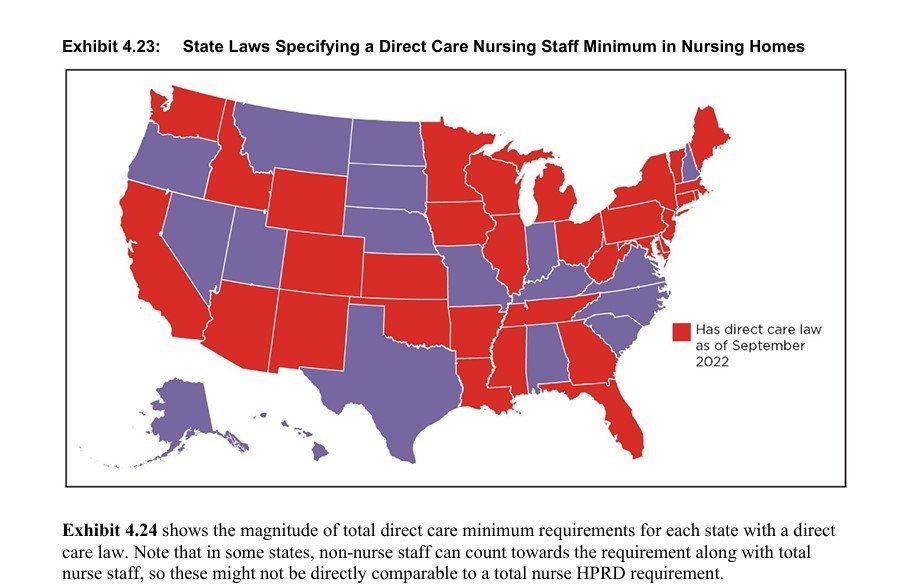
What's happening in the real world
CMS (Centers for Medicare & Medicaid Services) is expanding quality reporting requirements. Facilities must track and publicly report metrics on falls, infections, staffing levels, and resident satisfaction.
State attorneys general are increasingly investigating elder abuse and neglect cases. The enforcement environment has shifted from reactive to proactive.
Insurance companies are tying reimbursement to quality metrics. Facilities that can't demonstrate good outcomes face payment cuts.
Where this is heading
Transparency is the theme. Families can now access detailed quality ratings for nursing homes and assisted living facilities before making decisions. The days of information asymmetry are ending.
The compliance burden is real, especially for smaller facilities. Expect consolidation as operators who can't afford compliance infrastructure sell to larger chains.
12. Workforce Innovation Tackles the Staffing Crisis
With 99% of nursing homes reporting open positions, the industry is finally getting creative about workforce.
According to Bureau of Labor Statistics data via AHCA/NCAL, the average base salary for home health and personal care aides was $16.82 per hour as of May 2024. That's barely above fast food workers at $15.07/hour. Research shows 50% of direct care workers leave within the first year, primarily citing low wages.
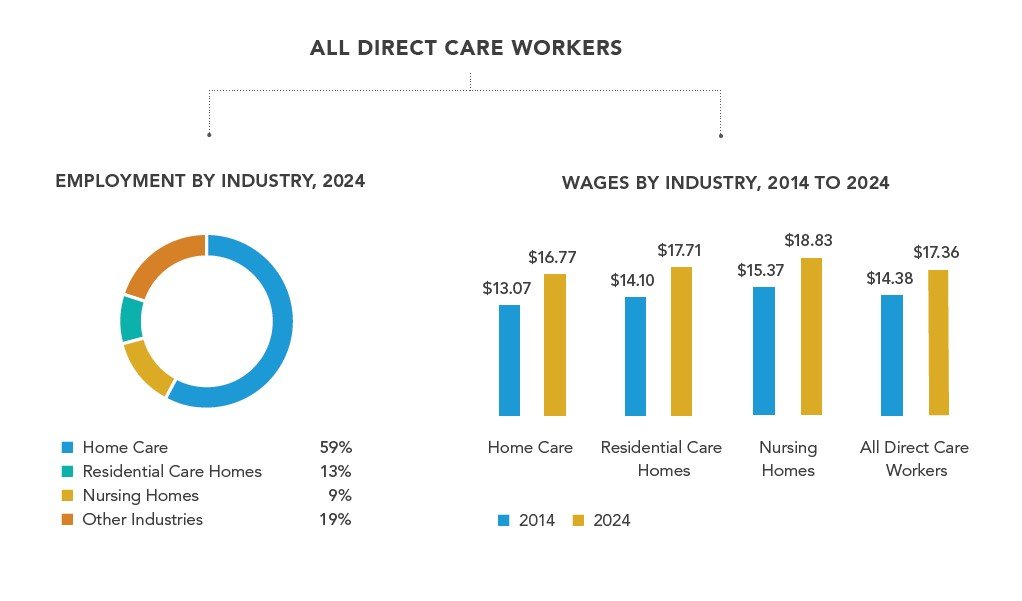
Source: Bureau of Labor Statistics Direct Care Worker Compensation Data 2024
But some organizations are proving that different approaches work. Higher wages, better training, career advancement paths, and technology that reduces administrative burden can dramatically improve retention.
The direct care workforce will need to fill 9.7 million total jobs between 2024 and 2034, according to PHI National research. That's not possible with current approaches.
What's happening in the real world
The SEIU and other unions are organizing caregivers and achieving wage increases in multiple states. Political momentum for higher caregiver pay is building.
Technology companies are building tools specifically to reduce caregiver documentation burden. Voice-to-text charting, automated scheduling, and AI-assisted care planning let caregivers spend more time with patients.
Immigration advocates are pushing for expanded visa categories for healthcare workers. Countries like the Philippines have trained nurses specifically for export; the U.S. could absorb far more than current quotas allow.
Where this is heading
The most innovative facilities are reimagining the job entirely. Instead of task-focused roles (bathing, feeding, medicating), they're building relationship-focused roles where consistent caregivers develop deep connections with small groups of residents.
The math is simple: if you can't hire enough people, you need each person to be more effective. That means technology, training, and job designs that reduce burnout and increase retention.
The Common Thread
Look across these twelve trends and a pattern emerges: senior care is being rebuilt from the ground up.
The old model — warehouse seniors in facilities, provide minimum required care, optimize for cost — is dying. Not because it's unpopular (though it is), but because it's economically unsustainable. We can't afford to institutionalize 73 million baby boomers.
The new model is distributed. Care happens at home, supported by technology, delivered by empowered caregivers, coordinated through unified platforms, and paid for through reformed insurance and government programs.
2026 is the year this transition becomes undeniable. The oldest boomers are turning 80. The technology is ready. The policy frameworks are evolving. The only question is which organizations will lead the transformation and which will be disrupted by it.
The companies thriving in this environment share characteristics: they design for seniors as primary users rather than afterthoughts. They integrate rather than fragment. They invest in caregivers rather than treating them as interchangeable. They leverage AI and automation to enhance human connection rather than replace it.
If there's one insight that spans all twelve trends, it's this: the future of senior care is personal. Personalized health monitoring. Personalized care plans. Personal relationships between caregivers and those they serve. The organizations that figure out how to deliver personalization at scale will define how we all age.
Want to spot emerging senior care trends before they hit mainstream? Check out our guide on how to identify market trends or explore what's gaining traction on our trends dashboard.



